JBC: A sugar-attaching enzyme defines colon cancer
Researchers have identified an enzyme that is absent in healthy colon tissue but abundant in colon cancer cells, according to a paper published in the Journal of Biological Chemistry.
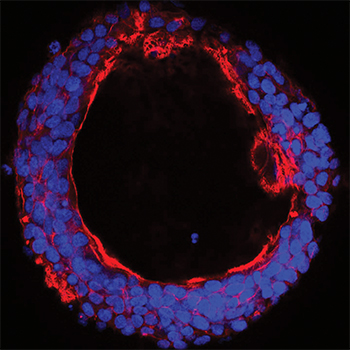 The enzyme GalNAc-T6 is upregulated selectively in colon adenocarcinomas, and its expression is associated with a cancerlike growth pattern.courtesy of Kirstine Lavrsen/University of Copenhagen
The enzyme GalNAc-T6 is upregulated selectively in colon adenocarcinomas, and its expression is associated with a cancerlike growth pattern.courtesy of Kirstine Lavrsen/University of Copenhagen
The enzyme appears to drive the conversion of normal colon tissue into cancer by attaching sugar molecules, or glycans, to certain proteins in the cell. Understanding the role that sugar-modified proteins play in healthy and cancerous cells is an emerging area of cancer biology that may lead to new therapies.
Hans Wandall’s team at the University of Copenhagen studied 20 enzymes that initiate the first step in a particular kind of glycan modification, called GalNAc-type O-glycosylation, found on diverse proteins. These enzymes, called GalNAc transferases, or GalNAc-Ts, are found in different amounts in different tissues, but their functions are poorly understood.
Wandall’s team, led by then-graduate student Kirstine Lavrsen, found that one of the GalNAc-Ts, called GalNAc-T6, was absent in healthy colon tissue but abundant in colon cancer cells. The team used CRISPR/Cas engineering of a colon cancer cell line with and without GalNAc-T6 to understand to which proteins the enzyme helped attach sugars and what effect this had on the cells.
“When we look at the 3D growth of a cancer cell line that has GalNAc-T6, it can form tubular structures with formation of something that looks like colon cancer tissue,” Wandall said. “When we take out GalNAc-T6, then suddenly the tissue formation changes to look more like the crypt structures that you would find in a healthy colon.”
Using mass spectrometry, the team categorized the proteins that GalNAc-T6 acted on in these cells.
“Our data suggest (that) this specific enzyme seems to affect a subset of proteins that could be involved in cell-cell adhesion,” Wandall said. In other words, the glycan modifications changed the patterns in which cells stuck together, leading the cells to develop as something that looked more like a tumor than a healthy tissue.
The next step is to understand precisely why adding sugars to the specific protein sites modified by GalNAc-T6 leads colon cells to develop abnormally. Glycan modifications can affect protein function in myriad ways. For example, they can make proteins that usually are cleaved into two unable to be cleaved, or prevent two proteins from binding to each other.
Wandall hopes that understanding glycosylation in cancer cells will lead to better early diagnostic tools, drugs or immunotherapies.
“Glycans add an additional context layer that could help us create more specific interventions,” he said.
“Glycans look so different in cancer compared to normal tissue, and it’s a really understudied field,” Lavrsen said. “There are a lot of things to be discovered.”
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Mitochondria shape kidney cell function
Researchers at the University of Washington, Seattle present the first quantitative comparison of mitochondrial interactomes between two epithelial cell types in the kidney.

Long-chain polyunsaturated fatty acids linked to postoperative delirium risk
Researchers show that altered lipid metabolism may contribute to postoperative delirium, a condition linked to increased risk for long-term cognitive decline. The study explores potential disease mechanisms, which have yet to be understood.

Glycosylation patterns across antibody isotypes distinguish tuberculosis states
Researchers at Taipei Medical University present the first site-specific glycosylation analysis of immunoglobulins in elderly tuberculosis patients.

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

Building a better model for drug delivery across the blood–brain barrier
Industry and academic scientists collaborated to develop a rat with humanized iron-transport receptors, enabling research into iron homeostasis and drugs that cross the brain’s barrier.

Fat synthesis enzyme crucial for milk fat and newborn growth
Researchers found that a deficiency of the fatty acid synthesis enzyme stearoyl-CoA desaturase-1 reduced mammary gland function during lactation and caused low birth weight in newborns that were fed milk from enzyme-deficient glands.

.jpg?lang=en-US&width=300&height=300&ext=.jpg)