To study Zika, they offered their kids. Then they were forgotten.
Rochelle dos Santos learned that her daughter would probably be born with microcephaly — a condition where a baby’s head is much smaller than expected — when she was seven months pregnant. It was 2016 and Brazil was going through an unprecedented microcephaly outbreak associated with the mosquito-borne virus Zika. After the baby was born and the diagnosis of congenital Zika syndrome was confirmed, several researchers approached dos Santos to see if she’d join relevant clinical studies. Eager to understand her daughter’s condition, she agreed.

in 2016 after dos Santos contracted Zika during her pregnancy in midwest Brazil.
Dos Santos says she was surprised to learn through a social media post last year that an international study that she participated in had been published in the journal Brain & Development. The study took over a year to be completed, and dos Santos had taken her daughter multiple times to the hospital for evaluations. As the head of an association for families of children affected by Zika in Goiás state in midwest Brazil, dos Santos wanted to share the findings with the other caregivers. She says she had to reach out directly to Hélio van der Linden, a neurologist at the Dr. Henrique Santillo State Center for Rehabilitation and Readaptation who authored the study in partnership with researchers in Brazil and the United States, to ask that a copy be shared with her. But she says he told her there was no point because it was written in English.
“Of course, we get upset,” she recalled in her native Portuguese. “We want to have this feedback and better understand this situation that is new for everyone.” Dos Santos — who noted that while she speaks only a little English, her husband reads and speaks English capably — said she feels used and that many other families share the same sentiment. “We know that Covid is now the priority," dos Santos adds, "but our children are still here, they still have needs."
The study’s author sent her the article, and dos Santos says her husband translated it for her — though she adds that she was also asked by van der Linden not to share it. (Van der Linden told Undark by email that while he did point out to dos Santos that the article was written in English, his main concern was running afoul of the journal's publishing rules. His request not to share it, he added, was for social media posts. “There was no problem in sharing the article with other mothers,” he wrote, “but I believe this wasn't clear to the mother of the patient.")
Children with congenital Zika syndrome face numerous health issues, all originating from the peculiar way in which Zika attacks the developing brain. In addition to the condition’s most pronounced feature — reduced head size — many have rigid muscles, difficulty swallowing and breathing, and problems with the retina and optic nerve, as well as other symptoms that are emerging as the children grow. “The doctors say that only time will tell how our children will be tomorrow,” dos Santos says, “because there are no adults with this syndrome.”
Dos Santos is not the only caregiver who felt left behind by scientists. Family groups like the one she heads have sprung up across the country, and members are increasingly at odds with the scientists who have used their children for research. The grandmother and caretaker of a boy with congenital Zika syndrome, Alessandra Hora dos Santos (no relation to Rochelle), launched one of these associations in Alagoas state in northeast Brazil in 2017. She says that lately she has been declining requests to participate in new studies — although such invitations are becoming rare because there haven’t been new outbreaks of the syndrome since 2016 — and she noticed that other families are doing the same.
Scientists who conducted the studies on Zika during the peak and the aftermath of the outbreak admit that communicating the results to families is not always effective, and that it was not the top priority during the Zika crisis. In the rush to collect data, not all researchers took the time to explain in detail what their projects were about and set clear expectations. Busy caretakers, on the other hand, were hardly able to carefully read the informed consent forms they were signing to authorize investigators to collect data from their children. Over the last few years, these families have demanded to participate more actively in the scientific discussion around Zika.
“We feel diminished,” says Alessandra Hora dos Santos. "It’s like we were lab rats. They come in nicely, collect information, collect exams on the child, and in the end we don’t know of any results. It’s like we are being used without even knowing why that is being done.”

Rochelle dos Santos helps her daughter with physical therapy. Many children
with congenital Zika disorder are physically disabled. |
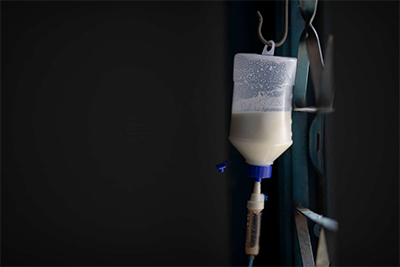
Due to difficulties swallowing, dos Santos’ daughter uses a feeding tube,
which is attached to her wheelchair. |
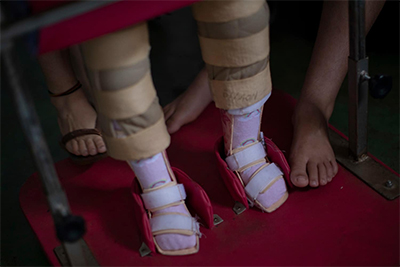
Dos Santos’ daughter uses leg braces to help her stand. Other symptoms
of the disorder are emerging as children grow. |

Dos Santos guides her daughter to create a finger painting. “Our children
are still here, they still have needs,” she says. |
By the time physicians started to notice a surge in microcephaly in Brazil in mid-2015, researchers had to scramble to design studies, get funding, and conduct analyses. Eventually, scientists from multiple institutions coalesced in the Microcephaly Epidemic Research Group (MERG). They began the research efforts even before the link with Zika had been established and had a crucial role in guiding public health strategies to tackle the epidemic. “There was a lot of pressure coming from the media and the health ministry,” says infectious disease expert Demócrito de Barros Miranda-Filho, a member of MERG and a professor at the University of Pernambuco. “We had to develop all the projects from scratch and submit them to the ethics committees within a deadline,” he says, adding that there was also pressure to give answers to the families.
One of the group’s concerns was to immediately share individual results of tests and clinical evaluations that could directly impact the child’s treatment. But when it comes to the general findings at the end of the study, says Miranda-Filho, the researchers didn’t properly communicate them to the participants.
“It is very complex to decode biological questions and put them into a more understandable language,” says Thália Velho Barreto de Araújo, an epidemiologist at the Federal University of Pernambuco and a member of MERG. “We haven’t figured out a way to do that yet, and we would need research resources to get advice for transforming technical language into something palatable.” Ricardo Arraes de Alencar Ximenes, an epidemiologist at both the University of Pernambuco and the Federal University of Pernambuco, notes that one of the obstacles to develop well-thought-out communication strategies is getting dedicated funding.
Physician Camila Ventura, one of the coordinators of an ambitious project with the goal of evaluating the neurodevelopment of about 200 children with congenital Zika syndrome over five years, says she is familiar with the families’ demands and agrees with them. But, there are other obstacles beyond adequate funding, she says. For example, with funding from the United States National Institutes of Health, the project is being developed at the Altino Ventura Foundation, a Brazilian health nonprofit, in partnership with the U.S. research organization RTI International. Because the project is done in partnership with other organizations, Ventura says it's not solely up to her to provide this feedback.
“This criticism applies to our own institution and I try my best to push for these answers” from our research partners, says Ventura. “The mothers see that we’re collecting data and they want to know: What about my kid?” she adds. “Is he getting better?”
Van der Linden wrote that when he invites a family to participate in a study, he tries to make it clear that the goal is to better understand the condition and that the findings might not benefit the participants themselves. “I explain that, after the study is done, there won’t be a ‘result’. Sincerely, I don’t offer or promise to call each one to explain the details, etc. I always make it clear that it is for science,” he wrote to Undark by email. “I believe there might have been an over-expectation, or an unrealistic expectation of something that was never promised.”
Soraya Fleischer, an anthropologist at the University of Brasília who coordinates a research project on the impact of Zika on the lives of families, says it’s also important to consider what these mothers mean when they ask for study results. “For the researchers, the result is what is published in a well qualified scientific journal or goes into their resume,” she says. But for the families, says Fleischer, sometimes the result is a simple blood test that confirms that the child’s disabilities were caused by Zika — an important document that grants access to certain social benefits reserved for children with the syndrome, which can be difficult to get via the public health system.
Not every parent has had a bad experience with Zika researchers. Jaqueline Silva de Oliveira, the mother of a 5-year-old girl with congenital Zika syndrome, says that whenever she needs these types of reports in order to claim social benefits, she reaches out to the scientist who enrolled her family in a genetics study. The girl’s twin brother was not affected by Zika, which caught the attention of a group at the Human Genome and Stem Cell Research Center at the University of São Paulo that wanted to try to identify potential protective genes.
“I participated to be able to help prevent other children from having microcephaly,” says de Oliveira. She says she can’t explain in her words what the results of the study were and she didn’t receive a document describing them. But overall, she thinks having participated in the study was a positive experience. She continues to have a connection with the researchers, and they helped her find a neurologist, one of the best in the state, she says, who managed to control her daughter’s epilepsy crises. “I helped the researcher on the study," she says, "and when I needed it, she helped me."
During the initial 2015 Zika outbreak and the years that followed, participation in the Brazilian Zika studies could be difficult. Luciana Lira, a medical anthropologist at the Federal University of Pernambuco, recalls accompanying two mothers to an event in 2018 in Recife, in Pernambuco state, one of the epicenters of the congenital Zika syndrome outbreak. The event was organized by a local university and an association for families of children with rare diseases. While the other mothers attended talks and participated in conversation circles, the mothers of children with congenital Zika syndrome were directed to a hall where researchers organized a task force to collect blood for a research project.
On that occasion, Lira says she watched while a nurse approached a mother to participate in the study. The mother “was so agitated that, when the nurse approached her and started explaining the study, she clearly wasn’t paying full attention because there were more urgent things to deal with. Her daughter was having a crying fit, she had to fix her feeding tube, all of that,” says Lira. “Then she agreed to participate, signed a paper and that’s it. This type of situation has become very commonplace.”
The researcher behind the project was Nilson Antonio de Assunção, a chemistry professor at the Federal University of São Paulo who was then studying the biochemical characteristics of blood among children with Zika. The study hasn't been published yet, de Assunção says, adding that he is aware that some families don't fully understand the purpose of his research when they agree to participate. "They get nervous because they are at an event, these are humble people, their children are crying and they end up not understanding very well what we’re explaining."
De Assunção says there isn’t much to be done about creating better strategies to communicate with families of children participating in studies. “I have been noticing this distrust in families,” he says, “but those who end up losing are the families themselves.” He says that he has previously tried to explain and educate the population about his work. “No matter what you do,” he adds, “there will always be this distrust.”
Lira and her colleagues have been observing the relationship between caregivers of children with Zika and biomedical scientists in Recife. Silvana Matos, also an anthropologist at the Federal University of Pernambuco, says that initially the caregivers welcomed the attention from scientists because they wanted to understand what had happened to their children. “The thing they complained the most about, right after this initial period,” she says, “was that the test results never came back to them and the researchers, from Brazil or abroad, never reached out again to tell them what happened.”
The families’ experiences with the medical trials made them wary of researchers more broadly. By the time the anthropologists started working with the families in late 2016, they had to redesign their work to deal with this research fatigue and gain trust, says Lira. The families “had been overwhelmed both by scientists trying to collect organic samples, and by journalists and researchers wanting to interview them,” says Fleischer. “There was an eagerness to learn what was happening” among the scientists and journalists, she adds, and the families “were the source.”
Lira spent several months following caregivers around before doing any interviews. Fleischer, who is not based in Recife, decided to come back to the city several times over the years to revisit the families and show them what had been produced with the data they had collected before — for example, an article or a newspaper story. Realizing that the caretakers were too busy to read long articles, Fleischer’s group created a blog to publish short stories about life with Zika that they would print out and distribute to the participants during their visits. The fact that the researchers kept coming back and reporting what they were doing made the families feel respected, according to Fleischer, and it was essential to build trust.

In Brazil, the ethical and legal framework for research involving human subjects was established in 1996 through a resolution by the Brazilian National Council of Health. To conduct a study involving human subjects in Brazil, researchers have to submit their proposal to a research ethics committee, much like in the U.S. Every research organization may constitute its own committee, which responds to the National Commission for Research Ethics (CONEP, by its Portuguese acronym).
Before entering a study, participants must sign a free and informed consent form, a document that describes the study, its goals, and possible risks and benefits of participating. According to the commission, the document should be written in clear and accessible language.
The need to share the findings with participants, which is at the core of the caregivers’ complaints, is not directly covered by the 1996 resolution. But the current ethical norms, in force since 2012, do state that research findings should be communicated to the community if there’s a potential to benefit the population, notes biologist Maria Mercedes Bendati, who retired from the municipal health department of Porto Alegre, in southern Brazil, in 2017 and is a CONEP member. “It already says that it is important to give this feedback,” she says. The next step, she adds, is to implement the requirement "and make it very clear in the academic education of the researchers that they should fulfill their social role, and know that the research implies giving these answers to the participants."
Bendati participated in the Pan American Health Organization Zika Ethics Consultation in April 2016, which originated an ethics guidance on key issues raised by the Zika outbreak.
Florencia Luna, the chair of the Zika Ethics Consultation, says the goal of the guidance was precisely to prevent situations like the ones the caregivers described. “We were very concerned about doing this research at that moment in the middle of the outbreak. So it’s a little bit like now, with Covid,” she says. “Even if you want to do [research] fast and quick, and you should do it like that, that doesn’t mean you have to avoid ethical standards.”
Luna, who is also the director of the bioethics program at the Latin American Faculty of Social Sciences in Argentina, believes that returning to the participants with the results is an ethical obligation. “Personally, I do think it is very important to come back and tell the good or the bad news,” she says, especially with Zika, which involves mothers and babies with health conditions. “At least to send them a letter, to call them on the phone,” she adds. “Maybe not to make them go to the clinic because it would be too burdensome for them, but there are other ways where you can communicate nowadays, with smartphones, with the internet.”
According to the International Ethical Guidelines for Health-related Research Involving Humans, a 2016 document prepared by the Council for International Organizations of Medical Sciences in collaboration with the World Health Organization, researchers “should engage potential participants and communities in a meaningful participatory process” which includes the dissemination of the study’s results.
Despite such guidelines, not communicating results to participants is seen by some researchers as business as usual. Carl Elliott, an expert in bioethics and a professor of philosophy at the University of Minnesota, says the situation narrated by Rochelle dos Santos, where the investigator hesitated to send her the study for which her daughter had collaborated, didn’t surprise him.
“If I were the research subject or the mother of the research subject, it would offend me and I think justifiably,” he says. “That said, I think the vast majority of research subjects don't do that sort of follow-up. They don't ask or are not even particularly interested in the papers.” Elliot says he doesn’t think the investigator gave the right response, but he imagines he was probably surprised by the request.
In any case, Elliott says he believes that, if a participant actively asks, the researcher must provide the results: “It's shameful that it takes so much effort, and often money, for the public to get access to the results of scientific studies published in the medical literature.”

In September 2018, the Brazilian caregivers’ discontent culminated at the annual Congress of the Brazilian Society of Tropical Medicine in Recife. That year, the program included several sessions about congenital Zika syndrome. According to a paper written by Lira, none of the families’ associations had been invited.
During one of the sessions on the main stage, Germana Soares, the mother of a boy with congenital Zika syndrome and the president of one of the largest family associations, requested to speak. She read aloud a letter to the event’s organizers. “We believe there is a lack of empathy and sensitivity to our reality, and a lack of respect in the fact that we were underestimated. As if we — the mothers, relatives, and caretakers — would lack the understanding to participate in a technical event to discuss a topic that is of our biggest interest,” the letter stated. “Are we mothers so ignorant, without the least bit of education, that we cannot understand a scientific article or a lecture. Or should the researchers be the ones to use a language that is more comprehensible? Are we totally wrong to demand a discussion about ethics in biomedical research? Are we just numbers?”
The organizers were apparently caught by surprise, as Soares’s speech wasn’t in the program. One of the speakers at the session called Sinval Pinto Brandão Filho, the president of the Society, to ask him what to do about it. He advised him to let Soares speak. “Our organization welcomes this debate with great satisfaction because we study the tropical diseases, in terms of controlling them” Brandão Filho says, adding that every year the Brazilian Society of Tropical Medicine invites patients of neglected diseases to a public forum during the congress to discuss the problems they face. “I see this as something specific that was immediately recognized that it should be more sensitively incorporated into the tribute session.”
Today, only sporadic cases of congenital Zika syndrome still occur, which makes it difficult to get funding for research, scientists say. The research focus has shifted to Covid-19, but the Zika health emergency might have left a legacy when it comes to research ethics.
“My personal reflection about the Zika experience in ethics committees is that perhaps there should have been a dialogue with the researchers to ask them how the findings would be shared with the participants,” says Bendati. “When it comes to Covid-19, the CONEP is now being very clear on the need for a proposal of feedback to be given to participants.” Learning from the mistakes of Zika might have contributed to this evolution, Bendati adds.
Luna says she’s aware that sometimes ethics are viewed as an obstacle to science. Tracking down the participants can be difficult, and researchers who might have moved on to another project often lack the time and the energy to pursue it. “But it’s part of what we have to do in order to build trust, to continue working,” she says. “If not, these women will not collaborate in any other research in their lives because they were disappointed.”
This article is republished from Undark. Read the original here.
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Glycosylation patterns across antibody isotypes distinguish tuberculosis states
Researchers at Taipei Medical University present the first site-specific glycosylation analysis of immunoglobulins in elderly tuberculosis patients.

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

Building a better model for drug delivery across the blood–brain barrier
Industry and academic scientists collaborated to develop a rat with humanized iron-transport receptors, enabling research into iron homeostasis and drugs that cross the brain’s barrier.

Fat synthesis enzyme crucial for milk fat and newborn growth
Researchers found that a deficiency of the fatty acid synthesis enzyme stearoyl-CoA desaturase-1 reduced mammary gland function during lactation and caused low birth weight in newborns that were fed milk from enzyme-deficient glands.

Flipping lipids and slime molds
A dull first job nearly pushed JBC associate editor Todd Graham out of science. Then a slime mold project changed his path. Now, he studies membrane biology and reflects on discovery, persistence and mentoring through uncertainty.

How smelling death alters worm behavior
Researchers have found that the roundworm C. elegans can smell death, and it changes how the worms behave, reproduce and age.

