More than ‘just a headache’
Most of us get headaches. Sure, it can be inconvenient, but you pop on a pain reliever and you’re fine within a few hours.
But have you or your loved ones experienced debilitating headaches that make it impossible to carry on with normal activities? What you might be experiencing or hearing about is “migraine” or “cluster headaches.”
Migraine is not just a headache. It is a neurological disorder, and headache is a primary symptom.

According to the National Headache Foundation, 40 million Americans suffer from migraine. World Health Organization statistics state that one in seven adults worldwide has migraines, and the experience is three times more common in women than in men.
How do you know if your headache is a migraine?
You can use the ID Migraine Tool by the National Headache Foundation.
-
Has a headache limited your activities for a day or more in the past three months?
-
Are you nauseated or sick to your stomach when you have a headache?
- Does light bother you when you have a headache?
Answering “yes” to two out of three of these simple questions effectively identifies migraine sufferers.
What is a migraine, and what causes it?
According to the Centers for Disease Control and Prevention, migraine is a complex neurological disorder. It often begins at puberty and mostly affects those people between the ages of 35 and 45.
It is more common in women, usually by a ratio of about 2:1, because of hormonal influences.
It is caused by the activation of a mechanism deep in the brain that leads to release of pain-producing inflammatory substances around the nerves and blood vessels of the head.
Stages of migraine
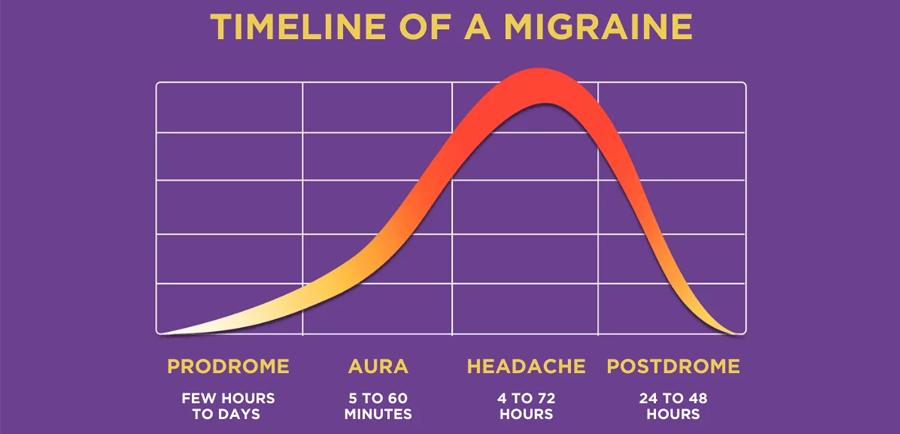
Migraine is complex and often occurs in different phases. According to Mayo Clinic, migraine can progress through four stages: prodrome, aura, attack and postdrome. It is important to note that the symptoms may not look exactly the same in everyone suffering from a migraine.
Prodrome — A few hours to few days before an actual migraine attack, one might start to experience some warning signs such as:
-
constipation
-
fluid retention
-
mood changes, from depression to euphoria
-
frequent yawning
-
increased urination
-
food cravings
Aura — The stage that follows the prodrome is the aura. According to Migraine Australia, about one-third of people with migraine experience an aura.
Auras could include the following symptoms:
-
visual phenomena, such as seeing various shapes, bright spots or flashes of light
-
vision loss
-
pins and needles sensations in an arm or leg
-
weakness or numbness in the face or one side of the body
-
difficulty speaking
Attack — An actual migraine attack can last anywhere between four hours to three days if left untreated. The frequency of attacks varies from one individual to another.
Symptoms during a migraine attack may include:
-
pain usually on one side of your head, but often on both sides
-
pain that throbs or pulses
-
sensitivity to light, sound, and sometimes smell and touch
-
nausea and vomiting
Postdrome —This phase is also referred to as a migraine hangover. After a migraine attack, one might feel exhausted and confused for up to a day. Some people report feeling euphoric.
Stigma associated with migraine
Migraine is often misinterpreted as just a headache. This undermines the complexity of the disease, which is a genetic, neurological disorder with dozens of unique symptoms.
According to the CDC, more than 70% of people will experience a tension headache in their lifetime; however, not all these headaches may be a sign of migraine.
Organizations such as the National Headache Foundation are playing a pivotal role in creating awareness about migraine.
Diagnosis and treatment
A neurologist should be able to diagnose a migraine based on physical examinations as well as by symptoms and medical history. In complex cases, one might need an MRI or a CT scan to identify the root cause of headaches, such as a tumor or brain damage.
Treatment for migraine mainly includes over-the-counter pain relievers as well as prescription medication such as Lasmiditan, Ubrogepant or opioid-based drugs.
Recent migraine research
Check out the following articles about migraine published in the American Society for Biochemistry and Molecular Biology’s open-access journals.
Identifying novel mechanisms involved in migraine development: The membranes of nerve cells contain voltage-gated calcium channels. It is known that mutations in the gene that encodes the α1-subunits of the Cav2.1 (P/Q-type) channels cause human diseases, including familial hemiplegic migraine type-1. In a study published in the Journal of Biological Chemistry, researchers examined how mutations in the β-subunits might also disrupt the functioning of calcium channels. They found that the mutations have profound effects.
Relationship between migraine and opioid-induced pain hyper-sensitivity: Opioid-based treatment is commonly used to treat migraine. However, continued use of opioid substances can result in increased pain sensitivity known as opioid-induced hyperalgesia. A recent study published in the journal Molecular & Cellular Proteomics screened for changes in more than 1,500 neuropeptides under these two conditions. Using liquid chromatography-mass spectrometry, the researchers identified 16 neuropeptides that were altered between the two conditions. Of those, pituitary adenylate cyclase-activating polypeptide (known as PACAP for short) was confirmed to act as a link between chronic migraine and opioid-induced hyperalgesia.
Involvement of a cell membrane protein in hemiplegic migraine: Hemiplegic migraine is a rare and serious type of migraine headache that affects one side of the body, resembling a stroke. Scientists have identified a mutation in the gene encoding a sodium–potassium pump involved in development of hemiplegic migraine. In a research article published in JBC, scientists described a mutation in the ATP1A2 gene, which encodes the α2 subunit of sodium–potassium pump. Briefly, sodium potassium pump helps neurons in the brain transmit signals using a flow of Na+ and K+ ions. This study provides insights about the characteristics of ATP1A2 mutations and offers a new perspective for the development, diagnosis and treatment of migraine and other neurological disorders.
More neurobiology coverage

Ebola virus hides out in brain: Monkeys treated with monoclonal antibodies fully recovered, but infection recurred.
What indirectly links brain disease to COVID-19? Armin Bayati, a JBC Herbert Tabor Early Career Investigator Award winner, presented his lab’s research at the ASBMB annual meeting in April.
Brain Awareness Week: An overview of current areas of exploration in brain science and disease. Topics include Alzheimer's, stroke, multiple sclerosis, traumatic brain injury, addition and more.
Brain research highlights: A special edition of “From the Journals” featuring recent brain research published in the American Society for Biochemistry and Molecular Biology’s open-access journals.
Faulty immune response may be behind lingering brain trouble after COVID-19: Headaches and trouble thinking plague some people after a coronavirus infection.
Brain wrinkles and folds matter: Researchers are studying the mechanics of how they form.
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Uncovering the molecular roots of fatty liver disease
Physician–scientist Silvia Sookoian discusses her path from hepatitis C care to MASLD research, her use of multi-omics to study steatotic liver disease, and how lipid metabolism and genetics are reshaping understanding of MASH and liver health.

Mitochondria shape kidney cell function
Researchers at the University of Washington, Seattle present the first quantitative comparison of mitochondrial interactomes between two epithelial cell types in the kidney.

Long-chain polyunsaturated fatty acids linked to postoperative delirium risk
Researchers show that altered lipid metabolism may contribute to postoperative delirium, a condition linked to increased risk for long-term cognitive decline. The study explores potential disease mechanisms, which have yet to be understood.

Glycosylation patterns across antibody isotypes distinguish tuberculosis states
Researchers at Taipei Medical University present the first site-specific glycosylation analysis of immunoglobulins in elderly tuberculosis patients.

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

Building a better model for drug delivery across the blood–brain barrier
Industry and academic scientists collaborated to develop a rat with humanized iron-transport receptors, enabling research into iron homeostasis and drugs that cross the brain’s barrier.