From the journals: JLR
Reversing alcoholism’s effects on lipid droplets. How HDL cholesterol might reduce COVID-19 risk. Shining light on the cholesterol–GPCR relationship. Read about recent papers on these topics in the Journal of Lipid Research.
Reversing alcoholism’s effects on lipid droplets
Alcohol-related liver disease, or ARLD, caused by chronic alcoholism is a major public health concern. An early sign of ARLD is fatty degeneration, or steatosis, which is caused by dysregulation of lipid metabolism and accumulation of lipids within the liver.
In a recent paper in the Journal of Lipid Research, Carol A. Casey and a team from the University of Nebraska and the Mayo Clinic explore the impact of chronic alcoholism on the function and composition of lipid droplets, or LDs, organelles in the liver that play a vital role in lipid metabolism and excess lipid storage. LDs consist of a phospholipid monolayer enclosing neutral lipids. This monolayer is also home to numerous proteins that regulate lipid metabolism — the LD proteome.
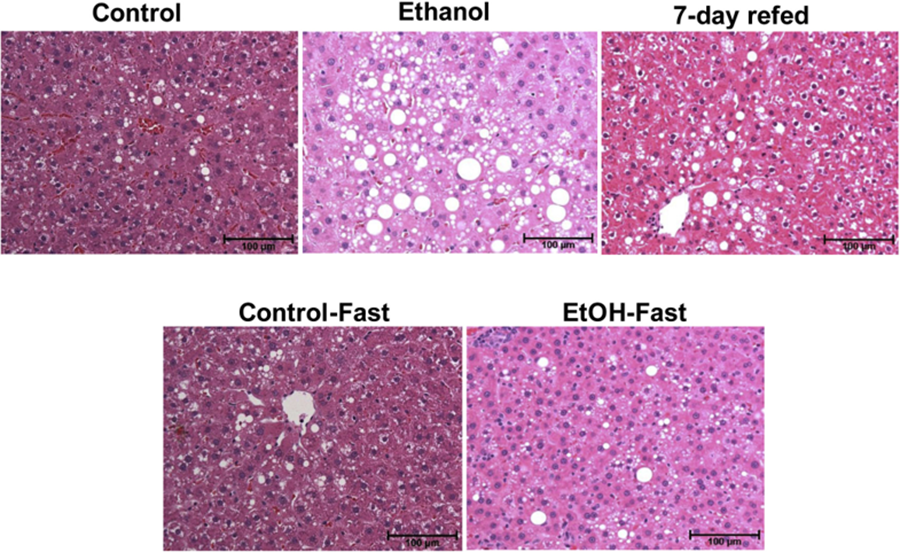
The researchers examined how feeding an alcohol-heavy diet to rats affected the composition of the LD proteome and whether subsequent replacement with a control diet over seven days (refeeding) or 48-hour fasting reversed the effects.
They observed that an ethanol-heavy diet led to a greater number and volume of LDs in liver sections as well as higher levels of triglycerides and nonesterified fatty acids, or NEFAs. Refeeding reversed these effects for both triglycerides and NEFAs. Fasting did so partially, albeit with NEFA levels similar to those resulting from the ethanol-fed diet.
Additionally, the levels of 388 LD proteins were altered with chronic alcohol intake, demonstrating a trend of reduced lipid utilization. For example, CIDEB, a protein known to induce LD fusion, was upregulated. This effect was reduced by both refeeding and ethanol fasting through recovering lipid utilization and mitochondrial function and reducing the levels of those proteins found to promote lipid accumulation. As Casey and the team wrote, “our data clearly support the notion that alcohol withdrawal, along with adequate nutritional support, is necessary for managing alcohol-induced liver injury.”
Increased HDL levels might reduce COVID-19 risk
Preexisting conditions that increase the risk of contracting SARS-CoV-2, the virus that causes COVID-19, have been a focal point in understanding the virus. Why these conditions increase risk is not well understood. In a recent paper in the Journal of Lipid Research, James R. Hilser, Yi Han and a team from the University of Southern California, the Cleveland Clinic and UCLA explore the connection between SARS-CoV-2 infection and biomarkers linked to preexisting metabolic conditions, such as obesity or coronary artery disease. The team compared high-density lipoprotein, or HDL, cholesterol and apolipoprotein A1, or ApoA1, levels in individuals who contracted the virus with data collected prior to the pandemic.
The findings indicate a connection between increased HDL cholesterol or ApoA1 levels and reduced infection rates. In people with high levels of these biomolecules, the reduced rate was as high as 20%. Hilser, Han and their team reasoned that this is potentially tied to immune-mediating properties of HDL cholesterol, writing, “HDL-cholesterol can protect against infections by a variety of pathogens, including bacteria and parasites, and can directly bind and neutralize various DNA and RNA viruses through ApoA1-mediated inhibition of viral fusion and entry into host cells.”
The sample size in this study was, however, too small to demonstrate a genetic link between HDL cholesterol levels and COVID-19 risk.
Shining light on the cholesterol–GPCR relationship
Cholesterol maintains structural integrity within cell membranes. Many G protein–coupled receptors, or GPCRs, require cholesterol. Researchers believe cholesterol allosterically binds GPCRs with high affinity and induces a conformational change favorable for endogenous ligand binding. This mechanism has not been explored fully, however.
In a new study in the Journal of Lipid Research, Laura Lemel, Katarzyna Nieścierowicz, M. Dolores García–Fernández and an international team developed an assay based on ion channel–coupled receptor technology to study the interaction between cholesterol and GPCRs. They examined the relationship in the context of the oxytocin receptor, OXTR, which mediates uterine contractions and lactation during and after pregnancy as well as playing a role in some social behaviors.
The team discovered that cholesterol and the GPCR ligand have a reciprocal relationship; ligand-bound OXTRs formed stable interactions with cholesterol even after cholesterol depletion. As the authors state, “New prospects arise for clearly identifying the binding site(s) of functional cholesterol molecules and for understanding the molecular mechanism of the dependence of OXTR on cholesterol, thanks to the possibility of selectively stabilizing the interaction of these molecules with the receptor.”
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Glaucoma model links immune signaling to disease progression
Researchers at Duke University determine genetic variations that could increase the risk of developing glaucoma.

Uncovering the molecular roots of fatty liver disease
Physician–scientist Silvia Sookoian discusses her path from hepatitis C care to MASLD research, her use of multi-omics to study steatotic liver disease, and how lipid metabolism and genetics are reshaping understanding of MASH and liver health.

Mitochondria shape kidney cell function
Researchers at the University of Washington, Seattle present the first quantitative comparison of mitochondrial interactomes between two epithelial cell types in the kidney.

Long-chain polyunsaturated fatty acids linked to postoperative delirium risk
Researchers show that altered lipid metabolism may contribute to postoperative delirium, a condition linked to increased risk for long-term cognitive decline. The study explores potential disease mechanisms, which have yet to be understood.

Glycosylation patterns across antibody isotypes distinguish tuberculosis states
Researchers at Taipei Medical University present the first site-specific glycosylation analysis of immunoglobulins in elderly tuberculosis patients.

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

