Scientists unmask a virus that mimicked human RNA and hit on a potential vaccine
Viruses are clever parasites that are quick to hack into host systems for their survival. But viruses can themselves be turned on their head. Can you imagine a virus hacking the immune system to hide from the body and then hacking the hacker itself to make a vaccine?
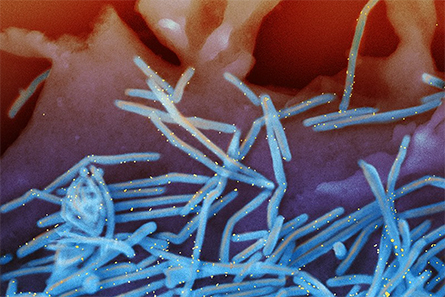
New research, published in February in Nature Microbiology, has shown that this is possible. Scientists determined that a virus called human metapneumovirus (hMPV) mimics human RNA to hide from the body's immune response. But blocking the ability of the virus to do so results in a mutant strain that can actually act as a candidate vaccine.
The human metapneumovirus (hMPV) was discovered in 2001. It is considered one of the leading causes of respiratory infections around the world, particularly in infants, elderly, and immunocompromised people. Although there have been many advancements in hMPV research since its discovery, there is still no Food and Drug Administration-approved antiviral or vaccine available to treat it.
hMPV uses RNA (a cousin of DNA) as a blueprint to make copies of itself. Several chemical modifications of RNA have been known for many years but only recently their roles have started to come to the surface.
Think of RNA modifications as do-it-yourself charms on a bracelet. You can add different decorations/charms to the chain (the RNA strand) that makes each bracelet unique. Similarly, human proteins modify their RNA to mark them with a unique identity that helps distinguish their own RNA from RNA belonging to foreign invaders like viruses.
A very common and important RNA modification is called m6A (N6-methyladenosine). M6A was discovered in the 1970s, but its biological function has largely been a puzzle for virologists. Imagine m6a as just one particular kind of charm on RNA's chain. As of now, there is no consensus on whether m6A positively or negatively affects viral load, or what it does for viruses.
In this new paper, led by Mijia Lu and Zijie Zhang from the Ohio State University Department of Veterinary Biosciences, researchers showed that the hMPV genome, anti-genome (template strand for RNA genome replication), and functional RNAs are festooned with m6A.
Next, the team moved onto understanding the function of these modifications. First, they identified which of hMPV's genes had the most m6A modifications. Then, they developed a mutated form of the virus that lacked these modifications so they could study how the virus performed without them.
To their surprise, they found that the mutant virus was less infectious, took longer to duplicate and synthesized less viral proteins in laboratory conditions than the original form, or the wild type, of hMPV. Encouraged by this discovery, the researchers then introduced the mutant virus into human lung cells (grown in a dish) and the eureka moment arrived. The mutant virus increased production of a protein called type I interferon (INF-1), an antiviral molecule made by the immune system, which is responsible for activating the first line of defense against pathogens.
This raised an important question: why would a virus with less m6A than normal activate a stronger immune response than the wild type virus?
Imagine a security system installed in your house. The security camera differentiates between family members and threats. Once a burglar is identified, the system alerts the owner of the potential threat. Similarly, humans have a built-in security camera that distinguishes between self (human) and non-self (viral, in this case) molecules. And once it detects non-self molecules, it activates the alarm to release INF-1, which calls for help from other immune cells, including T-cells and antibodies.
The scientists deduced that the extra m6As on the RNA of the wild type virus effectively disguised it as human RNA (self-RNA). The virus is quite clever. It gains m6As on its RNA that make it look human, tricking the body's security camera and decreasing the likelihood that the virus is destroyed it before its too late.
Without the modifications in viral RNA, the immune system is no longer confused and can effectively mount a defense strategy. The researchers confirmed this by conducting an experiment in rats infected with the mutant virus. They observed that the rats immunized with the mutant virus and then infected with wild type hMPV produced more IFN-1 and a higher antibody and T-cell immune response compared to rats that were not immunized. This means that the mutant virus can effectively provide complete protection against the viral infection.
This pivotal experiment proved to be the last piece of the puzzle confirming that genome editing to mutate modification sites in the virus can serve as an effective strategy to design novel vaccines against hMPV. hMPV has an infection rate of 3.8% in children, making it incidence similar to that of influenza virus. And the estimated annual burden associated with hMPV infection is 55 clinic visits and 13 emergency department visits per 1000 children – proving it a substantial health care concern.
This research is an excellent reminder that though viruses are a global health threat, they still serve as great teachers of cell biology. And these teachers will continue to provide scientists with valuable tools to gain deeper insights into the world of RNA modifications.
![]()
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Glaucoma model links immune signaling to disease progression
Researchers at Duke University determine genetic variations that could increase the risk of developing glaucoma.

Uncovering the molecular roots of fatty liver disease
Physician–scientist Silvia Sookoian discusses her path from hepatitis C care to MASLD research, her use of multi-omics to study steatotic liver disease, and how lipid metabolism and genetics are reshaping understanding of MASH and liver health.

Mitochondria shape kidney cell function
Researchers at the University of Washington, Seattle present the first quantitative comparison of mitochondrial interactomes between two epithelial cell types in the kidney.

Long-chain polyunsaturated fatty acids linked to postoperative delirium risk
Researchers show that altered lipid metabolism may contribute to postoperative delirium, a condition linked to increased risk for long-term cognitive decline. The study explores potential disease mechanisms, which have yet to be understood.

Glycosylation patterns across antibody isotypes distinguish tuberculosis states
Researchers at Taipei Medical University present the first site-specific glycosylation analysis of immunoglobulins in elderly tuberculosis patients.

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

