From the journals: JLR
Linking a STEAP-3 boost to liver disease. How two drugs break down cholesterol. Seeking diagnostics for a rare birth condition. Read about papers on these topics recently published in the Journal of Lipid Research.
Linking a STEAP-3 boost to liver disease
Roughly one-quarter of the world’s adults suffer from nonalcoholic fatty liver disease, or NAFLD. This condition, which can progress from a simple fatty liver to severe scarring, or cirrhosis, and even liver cancer, does not yet have a cure.
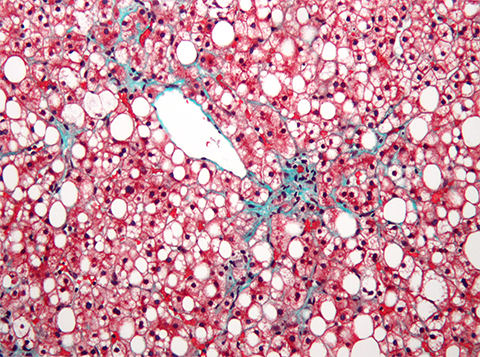
However, recent studies suggest some molecular targets for future medications. Take the metalloreductase called six-transmembrane epithelial antigen of prostate 3, also known as STEAP3. This protein plays an outsized role in biological processes from cell division to inflammation and cell death — as well as liver diseases.
Recently, Ting Ding, Siping Chen and Wenchang Xiao, along with a team from Huanggang Central Hospital in China, discovered that STEAP3 increases in NAFLD. Their study in the Journal of Lipid Research suggests how this ubiquitous protein may influence the trajectory of the disease and how future investigators might design an effective drug to counter it.
First, the scientists found that STEAP3 levels rise in lipid-rich hepatocytes, or liver cells, from an obese mouse model or NAFLD tissue. They further determined that STEAP3 promotes lipid buildup in hepatocytes.
Comparing knockout mice (missing the STEAP3 gene) with a wild-type control group, the team learned that the absence of STEAP3 led to lower body weights, fasting blood glucose and serum insulin levels — plus better glucose tolerance. These results emerged after 24 weeks of a high-fat diet for both groups of mice. Assays confirmed that the absence of the STEAP3 inhibits formation of glucose.
The mice without STEAP3 also tested lower for several key health measures, from liver weight to total cholesterol. Taken together, these results showed that the absence of STEAP3 diminished NAFLD in the mice. In this way, the study offers a crucial, novel finding: STEAP proteins help govern the development of NAFLD.
In addition, the team’s experiments suggested that STEAP3 interacts with transforming growth factor beta-activated kinase 1, or TAK1, along the mitogen-activated protein kinase, or MAPK, signaling pathway in hepatocytes.
How two drugs break down cholesterol
Avoiding atherosclerosis, the buildup of fatty plaque along inner artery walls, requires efficient routing of cholesterol for the breakdown in the liver, a process known as reverse cholesterol transport. High-density lipoprotein, or HDL, cholesterol helps rid the bloodstream of the low-density lipoprotein, or LDL, cholesterol that heightens the risk of heart attack or stroke.
Yet, scientists still do not fully grasp how two cholesterol ester transfer proteins, or CETP, inhibitors, dalcetrapib and anacetrapib, help drive cholesterol to the liver, splitting it into HDL particles. Early clinical trials failed to show promise, but a recent trial found that anacetrapib lowered cardiovascular events by 9%.
Mathieu Brodeur and David Rhainds of the Montreal Heart Institute and a team of scientists in Canada and Switzerland looked at how CETP inhibitors effect HDL in rabbits and humans. Their study appeared in the Journal of Lipid Research.
In rabbits already getting atorvastatin, a drug commonly used to treat high cholesterol and triglycerides, the inhibitors raised levels of HDL. In the human subjects, dalcetrapib boosted concentrations of large HDL particles and apolipoprotein (apo) B-depleted plasma apo E, eventually producing apo E-containing HDL without apo A-I.
The research suggests that the LDL receptor may be vital to the breakdown of these complex molecules. Specifically, CETPi spurs the production of large apo E-containing HDL byproducts, without apo A-I. The resulting particles may play a key role in reverse cholesterol transport, without CETP involvement, in the transfer of HDL to apo B-bearing lipoproteins.
Seeking diagnostics for a rare birth condition
In a hospital delivery room, parents are preparing to welcome their new baby. However, the infant emerges with taut, scaly skin and turned-out lips and eyelids. The medical team diagnoses a genetic disease: autosomal recessive congenital ichthyosis, or “collodion baby.”
Infants with this condition are at higher risk of microbial infections, fluid loss, electrolyte imbalance and pneumonia, among other complications. Physicians cannot yet predict whether the disease will be self-healing and vanish within the first year of life or lead to lifelong itchy skin and other symptoms.
Now researchers in Japan have fresh findings that could point the way toward making that prediction and helping parents plan the best care for their child.
The case studies reported in the Journal of Lipid Research by Takuya Takeichi of the dermatology department of the Nagoya University Graduate School of Medicine and colleagues involved two self-healing patients from different families — one infant with no family history of similar disease and one 11-year-old with a family history of skin disorders.
The researchers found through genetic sequencing that both children had mutations in the CYP4F22 gene. The team then focused on a group of lipids, the ceramides, which play crucial roles in the outer layer of human skin, the stratum corneum.
The researchers used a special tape to take skin samples from the children, the infant’s parents and people without the condition. Through a lipid analysis, the team found lower levels of acylceramides in the children than in the parents and others without the condition.
In the future, the scientists concluded, noninvasive lipid tests and genetic testing in combination could provide parents and health care providers with vital information for treatment plans.
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Blood glycome possibly predicts lifespan
Researchers at the University of Santiago de Compostela show that total serum N-glycome can predict mortality independent of traditional risk factors.

Building a better model for drug delivery across the blood–brain barrier
Industry and academic scientists collaborated to develop a rat with humanized iron-transport receptors, enabling research into iron homeostasis and drugs that cross the brain’s barrier.

Fat synthesis enzyme crucial for milk fat and newborn growth
Researchers found that a deficiency of the fatty acid synthesis enzyme stearoyl-CoA desaturase-1 reduced mammary gland function during lactation and caused low birth weight in newborns that were fed milk from enzyme-deficient glands.

Flipping lipids and slime molds
A dull first job nearly pushed JBC associate editor Todd Graham out of science. Then a slime mold project changed his path. Now, he studies membrane biology and reflects on discovery, persistence and mentoring through uncertainty.

How smelling death alters worm behavior
Researchers have found that the roundworm C. elegans can smell death, and it changes how the worms behave, reproduce and age.

A chance encounter with the lab
Payton Stevens never planned to become a pancreatic cancer researcher. A temporary job set him on a path from rural Kentucky to leading research on Wnt signaling and metastasis, where he now pairs discovery with mentorship and science advocacy.

