JLR: New insights into treating amoebic keratitis
The human body provides a hospitable environment for many micro-organisms that are essential to our survival. At the same time, it also attracts a host of parasites that, if not treated properly or eradicated, can be extremely harmful to our health. One such class of parasite is the infective amoeba, which causes rare and sometimes fatal diseases in humans. The Acanthamoeba species, found worldwide, mostly in water and soil, causes amoebic keratitis, or AK — an eye infection of the cornea that can result in permanent blindness. In the USA, 85 percent of AK cases occur in soft contact lens users. Although AK is potentially life-threatening, its treatment is not yet promising, owing to drug resistance and the absence of species-specific drugs. Hence, we need to identify specific drug targets to better fight these parasites.
Designing species-specific drugs requires an understanding of the unique evolutionary differences among species, especially with respect to biochemical pathways responsible for the survival of the parasite within the host. The Acanthamoeba life cycle has two stages — cyst and trophozoite. The trophozoite is the active form that infects humans, while the cyst is the dormant form that can survive harsh conditions such as stress and lack of nutrients. When conditions become favorable, the cyst transforms to a trophozoite via a process called excystment. Both forms can enter the human body through wounds, nostrils or contact with water.
 Electron micrographs show the two stages in the life cycle of Acanthamoeba castellani. Courtesy of the W. David NES labORATORY
Electron micrographs show the two stages in the life cycle of Acanthamoeba castellani. Courtesy of the W. David NES labORATORY
Certain metabolic pathways cause the Acanthamoeba to cycle between stages and help the infective trophozoites survive and proliferate in humans. Thus, targeting these specific pathways could prove to be an efficient strategy to treat Acanthamoeba infections. W. David Nes and his group at Texas Tech University have investigated such pathways and reported sterol C24-methyltransferases, or SMTs, synthesized only in amoebae, as novel druggable targets. Their findings were published in the Journal of Lipid Research.
Sterols are amphipathic molecules that, by virtue of their lipid-based properties, act as membrane inserts to control overall growth and development. Ergosterol biosynthesis has been established as essential for the survival of many amoebae in humans, and SMTs are critical enzymes in the ergosterol biosynthesis pathway. SMTs catalyze a crucial step in the ergosterol pathway that maintains trophozoite growth. Interestingly, SMTs are absent in humans. Thus, the researchers found that inhibiting these enzymes with transition-state analogs that blocked the catalytic site on the enzyme, or with suicide substrates that irreversibly bound covalently to the enzyme, stopped the growth of trophozoites but had no effect on normal cholesterol biosynthesis in human cells. So this approach could treat specifically Acanthamoeba infections without harming us. This is the highlight of Nes’ published work.
The work has been quite challenging, especially because differences in sterol biochemistry and life-cycle events among amoeba species make it hard to identify common drug targets. Moreover, Nes’ group required an extensive collaboration to integrate a multidisciplinary approach so as to provide “the most effective drugs, which would escape mechanisms that otherwise could compromise their therapeutic longevity,” Nes said.
Having used keratitis-causing Acanthamoeba castellanii as the model system in their published study, Nes and his group now want to test their hypothesis in mouse models. They also plan to extend their inhibitor studies to Naegleria fowlerii, a “brain-eating amoeba” that can cross the blood-brain barrier and destroy brain tissue, resulting in a disease called primary amoebic meningoencephalitis, or PAM. Further down the road, they hope to develop high-throughput screening techniques to repurpose existing drugs as novel SMT catalysis inhibitors to cure amoebic infections.
 Isha Dey is a Ph.D. candidate at Rosalind Franklin University of Medicine and Science.
Isha Dey is a Ph.D. candidate at Rosalind Franklin University of Medicine and Science.Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Fat synthesis enzyme crucial for milk fat and newborn growth
Researchers found that a deficiency of the fatty acid synthesis enzyme stearoyl-CoA desaturase-1 reduced mammary gland function during lactation and caused low birth weight in newborns that were fed milk from enzyme-deficient glands.

Flipping lipids and slime molds
A dull first job nearly pushed JBC associate editor Todd Graham out of science. Then a slime mold project changed his path. Now, he studies membrane biology and reflects on discovery, persistence and mentoring through uncertainty.

How smelling death alters worm behavior
Researchers have found that the roundworm C. elegans can smell death, and it changes how the worms behave, reproduce and age.

A chance encounter with the lab
Payton Stevens never planned to become a pancreatic cancer researcher. A temporary job set him on a path from rural Kentucky to leading research on Wnt signaling and metastasis, where he now pairs discovery with mentorship and science advocacy.

Light-activated small molecule could transform eye infection treatment
Contact lenses raise the risk of infectious keratitis, a leading cause of blindness worldwide. A biotech company is commercializing a light-activated therapy using a ROS-generating molecule to rapidly kill microbes in the cornea to preserve vision.
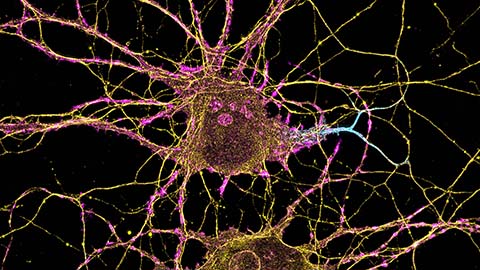
The molecular orchestra of memory
Calcium, calmodulin and calcium/calmodulin-dependent kinase II form a molecular axis that turns fleeting neural activity into lasting memories. New research shows how memories are stabilized, and possibly even protected or repaired.

