An entrepreneur fights disease on the ground
Imagine a small rural community most of a day’s walk from the nearest clinic. A community health worker comes through town, vaccinating local children, giving prenatal vitamins to expectant mothers, and offering tests for infections like HIV and malaria. With a type of diagnostic device that resembles a home pregnancy test, the worker, often a volunteer, can do a blood test quickly, far from the lab.
 Paula Fernandes and a training course participant look at tools for laboratory supply chain management. Courtesy of Global Scientific Solutions for Health
Paula Fernandes and a training course participant look at tools for laboratory supply chain management. Courtesy of Global Scientific Solutions for Health
Such tests are simple and should be easy to use, but they have pitfalls. A recent study found that single-use vials of buffer packaged with some tests can leak, and substituting water or saline may give a false-positive result. Paula Fernandes, who trains health care workers around the world, recently saw someone apply a blood sample to the wrong end of a diagnostic device.
Rapid diagnostic tests “are said, and believed, by many in the public health sector to be easy-to-use and reliable,” Fernandes said. “And yes, if used and stored and managed correctly, they are reliable. But there are so many areas where quality is degraded.”Fernandes started her company, Global Scientific Solutions for Health, to solve quality problems in the clinical lab. She and her team consult with ministries of health and train lab workers and health care providers around the world to make sure diagnoses are reliable and patients get the care they need.
An unusual path to a Ph.D.
Fernandes’ passion for science began early. “When I was 8, I decided I was going to be a microbiologist,” she said.
Her father, who ran a small business in England installing refrigerators, took her with him to work during summer holidays. One year, he brought her to a lab that needed a new cold room.“My eyeballs must have been so big walking into this lab,” Fernandes said. “Someone took me and showed me — I don’t know, a wheat germ or something under the microscope. I was like, ‘Wow. There is a whole hidden world that I never knew anything about, and it’s incredible.’”
For her birthday that year, her family gave her a microscope, and she dissected everything she could find. But there was one obstacle to becoming a microbiologist. “I really hated school. The only thing I liked about school was biology.”
Fernandes dropped out at age 15, later returning to take exams for the general certificate of secondary education, or GCSE. In the United Kingdom, these tests usually are taken at the end of 10th grade. At the time, they marked the end of compulsory education; some students went on for two more years of schooling followed by exams known as A-levels. But Fernandes was impatient to get out of high school and into the lab.
While preparing for the GCSEs, “I started hand-writing letters to laboratories all over the southeast of England,” she said. “I can’t remember how many letters I wrote, but I know my hand hurt.”
She sent dozens of inquiries for entry-level work, received two replies and landed a job in the microbiology lab at a general hospital in northwest London.
The work was poorly paid, and one of her least favorite tasks was spending hours autoclaving blood cultures used to diagnose infections and sluicing them down drains. But Fernandes was thrilled to be in a real lab with real bench work going on nearby. She was especially fascinated that her co-workers sniffed agar plates to detect certain microbes.
“I was a bit of a busybody when it came to science. I was always at the bench asking questions,” she said. Her fascination was clear to her co-workers. “People started teaching me stuff. I had a good nose: I was able to sniff out Haemophilus influenzae on a plate of Pseudomonas.”
Sensing potential, her manager sent her for a certification course in medical laboratory science.
Around that time, an aunt was diagnosed with an advanced case of tuberculosis. Fernandes was shocked when the infection, which she diagnosed in the lab but thought of in strictly historical terms, eventually killed her aunt.
“I was there with the entire family around her bedside when she died,” she said. “It was a case of basically turning off the life support ... I remember thinking to myself, ‘How can a disease like tuberculosis kill my aunt right in front of my eyes when she’s not even 40?’ She had other problems that made her more susceptible — but (until late in the infection, her TB) wasn’t diagnosed! It wasn’t picked up! How could it not have been diagnosed? I couldn’t understand this. That had a huge impact on me.”
Meanwhile, her professors in the medical lab science program encouraged Fernandes to continue her education. Because she hadn’t taken the A-level exams, applying to university was a tricky proposition. The professors in her program at Paddington College petitioned the national university entrance board for an exception, enabling her to go on for a bachelor’s in biotechnology. She excelled, and she later was accepted into graduate school at Cambridge University.
“I went from this rough, rebellious kid to somebody who was doing a Ph.D. in genetics at Cambridge,” Fernandes said. “And Cambridge was funny, because I don’t think they had anyone like me … There’s this whole background that I was missing, but I also felt like people were kind of interested in me because of that.” Fernandes wrote her dissertation on mycobacterial genetics and planned for an academic career researching tuberculosis.
Diagnosing diseases in humans
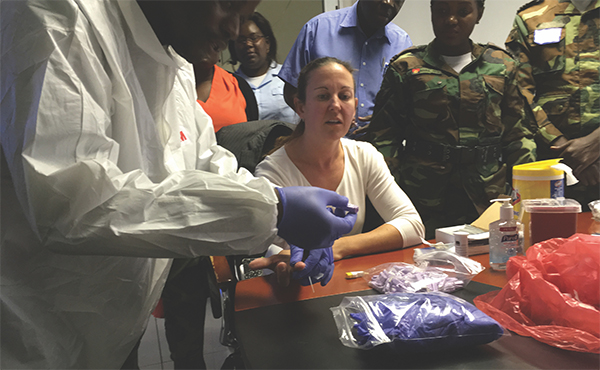 Paula Fernandes demonstrates fingerstick blood sample collection to military laboratory workers in Angola. Courtesy of Paula Fernandes
Paula Fernandes demonstrates fingerstick blood sample collection to military laboratory workers in Angola. Courtesy of Paula Fernandes
In 2001, Fernandes moved to the U.S. for a postdoctoral fellowship in Baltimore. After a few years and a change in labs, it became clear that she didn’t want to be a research professor.“I felt that there was too much distance between proteins that I was working on and my old life diagnosing diseases in humans, which seemed far more exciting to me,” she said.
She returned to the clinical laboratory just as molecular diagnostics were becoming available commercially, prompting a change in how clinical labs worked. After a year at a clinical pathology laboratory back in England, Fernandes returned to the U.S. for personal reasons. She interviewed for a job helping to launch laboratories as part of the President’s Emergency Plan for AIDS Relief. She knew the job was in Africa, but the hiring manager didn’t tell her exactly where, and she didn’t think to ask. That didn’t put her off.
“I was like, ‘Oh, I want to go to Africa and help set up labs there,’” she said. “I had just done that at a lab in the U.K., and I thought it was really interesting.”
Country X turned out to be Nigeria. After a few years helping to set up diagnostic and toxicity monitoring labs there, Fernandes became a program manager at the Association of Public Health Laboratories, based in Maryland, and enrolled in an MBA program. As she moved up in the ranks and away from the field, she said, “I realized that the lab was never at the forefront of everyone’s mind doing public health. Yet it was the lab that determined whether there was a public health issue or not.”
That realization motivated Fernandes to found her company, Global Scientific Solutions for Health, in 2008. “For me, there was just too big a gap between the policy and the practice,” she said. “I started GSSHealth because I really wanted to focus on the field and focus on bridging that gap.”
She describes the company’s work as “putting policy into practice”: implementing the decisions of health policy makers in developing countries that don’t have unlimited funds to throw at public health problems.
“The starting point is always global health policy and international health regulations,” Fernandes said. “Let’s say, for example, ‘If you have HIV, you need to have a viral load test.’ That would be a policy statement … Then it’s a question of actually making it happen.”
This viral load testing policy is a real one, recommended by the World Health Organization and its partners in 2013. However, with logistical and technical concerns, enacting the policy worldwide is a Herculean effort. If no clinical labs are available, if lab workers lack the tools or training to conduct a viral load test, or if reagents or equipment maintenance don’t arrive reliably, then “give each patient with HIV a viral load test” becomes an impossible instruction.
Fixing these problems in collaboration with local health care providers, health ministries and nongovernmental organizations is where Fernandes and her team come in. They offer training to lab technicians, trainers, auditors, community health workers and others in the healthcare system, working to strengthen existing systems rather than duplicating them. The team focuses in particular on regions far from national reference labs in countries’ capitals.
“The places that are most vulnerable to public health events and biosecurity events (are) places on borders between countries,” Fernandes said, citing the 2014 Ebola outbreak in West Africa and work GSSHealth and its partners have done on implementing interventions to reduce antimalarial resistance at the border between Thailand and Cambodia. “There’s a lot of travel back and forth; there’s a lot of mixing of populations and diseases. These are very important areas.”
The company has 10 employees at its office in the heart of Baltimore as well as subject matter experts in Africa and Southeast Asia. “We’re really mission-driven here,” Fernandes said. “Passion is infectious. We may have a small team, but every person here is just fantastic, and you’re nothing without that.”
Advice for aspiring entrepreneurs
Paula Fernandes offers these recommendations for scientists interested in starting their own businesses:
Ask questions. Go to networking events and meet people. “I think it’s really important just to get some exposure just on the language, on the philosophy. Speak to entrepreneurs and find out their path, because it’s always fascinating.”
Be adaptable. Fernandes transitioned “from being a scientist who’s focused on a very specific technical problem like quality diagnostics to hiring, managing people and having to handle things like IT … You think you’re a microbiologist? Well, now you’re putting the trash out, making the tea, you’re the HR person, you’re the IT person, you’re the bookkeeper — OK, we have a bookkeeper and accountant, but still — and you’re the contracts manager.” She faced a steep learning curve figuring out how to handle everything.
Take advantage of training opportunities. For younger scientists interested in starting a business, Fernandes recommends starting to practice and learn about the path as early as possible. As a graduate student at Cambridge, she entered a competition called the Biotech Young Entrepreneurs’ Scheme. “I think that was the seed that really made me want to start my own company.”
Do what you know … and love. After competing in BiotechYES, Fernandes spent time looking at possible ventures. But then, “It suddenly occurred to me, why am I trying to start a business in something other than what I already do? … I’m right here, I know what it is I’m doing right now, I know what I could do to improve it … and it’s the one thing on earth I’m most passionate about.”
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Industry
Industry highlights or most popular articles

How Alixorexton could transform narcolepsy treatment
A new investigational drug, alixorexton, targets the brain’s orexin system to restore wakefulness in people with narcolepsy type 1. Alkermes chemist Brian Raymer shares how molecular modeling turned a lab idea into a promising phase 3 therapy.

Inside industry postdocs
As more Ph.D. scientists look beyond academia, industry postdocs offer a new kind of training, where mentorship meets mission-driven research. Fellows at Pfizer and Genentech share how these programs prepare them to translate discovery into impact.

Black excellence in biotech: Shaping the future of an industry
This Black History Month, we highlight the impact of DEI initiatives, trailblazing scientists and industry leaders working to create a more inclusive and scientific community. Discover how you can be part of the movement.

Attend ASBMB’s career and education fair
Attending the ASBMB career and education fair is a great way to explore new opportunities, make valuable connections and gain insights into potential career paths.

Benefits of attending a large scientific conference
Researchers have a lot of choices when it comes to conferences and symposia. A large conference like the ASBMB Annual Meeting offers myriad opportunities, such as poster sessions, top research talks, social events, workshops, vendor booths and more.

Biotech startup worms its way into therapeutics
Andrea Choe's company, Holoclara, has created an anti-inflammatory drug based on a molecule from worms.

