MCP: Catching ovarian cancer when it’s curable
Fewer than half of ovarian cancer patients survive for five years after their diagnosis. According to the American Cancer Society, this is because only about one-fifth of ovarian cancer cases are detected early, when the chances of successful treatment and recovery are highest.
“If we could change this reality by detecting (ovarian cancer) at a curable stage, we could save many lives,” said Keren Levanon, a physician-researcher at Chaim Sheba Medical Center in Israel.
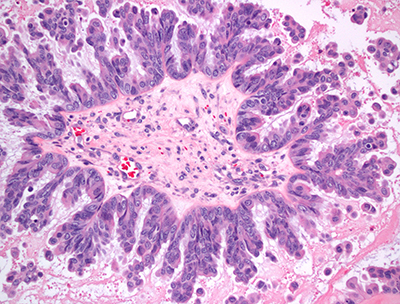 A section of an ovary stained with hematoxylin and eosin, showing a roughly star-shaped tumor. This tumor can be identified as aggressive because of its micropapillae, or outgrowths.Virginia Commonwealth University
A section of an ovary stained with hematoxylin and eosin, showing a roughly star-shaped tumor. This tumor can be identified as aggressive because of its micropapillae, or outgrowths.Virginia Commonwealth University
In the journal Molecular & Cellular Proteomics, researchers led by Levanon and Tamar Geiger of Tel Aviv University report a new test for ovarian cancer that outperforms previous tests. They hope it can be used to screen women who are genetically predisposed to the disease.
The researchers searched for signatures of cancer in uterine fluid sampled by liquid biopsy during surgery. They compared samples from women with ovarian cancer who had surgical treatment and from volunteers who had gynecological surgery for reasons unrelated to cancer, such as uterine fibroids or benign ovarian cysts.
Bodily fluids contain many proteins. Strong signals from the most common proteins can mask signals from smaller amounts of cancer-linked proteins that also might be present. To overcome that difficulty, researchers isolated microvesicles from the uterine fluid. Because microvesicles are shed from cells, they contain almost none of the signal-masking blood plasma proteins. Instead, they contain protein cargo that may vary between normal and malignant tissues.
Using proteomics, the researchers compared thousands of proteins in uterine microvesicles from 12 healthy volunteers and 12 cancer patients. Then they used machine-learning algorithms to search for patterns of protein abundance that differed among the samples.
“We developed a diagnostic set of nine proteins that distinguishes women with ovarian cancer from healthy women with greater sensitivity and specificity than reported before,” Levanon said.
The researchers then tested the set’s accuracy in 152 women, 37 of whom were known to have ovarian cancer. The test had 70 percent diagnostic sensitivity, meaning that it correctly detected cancer in 25 of the 37 study participants who truly had cancer, including all early-stage cases; it also had 76 percent specificity, meaning that it correctly identified about three out of every four healthy volunteers as healthy. It outperformed previous proteomics-based tests, which had less than 60 percent sensitivity.
Though the study used fluids collected during surgery, the proteomic test can also be run on samples collected in a minimally invasive procedure similar to intrauterine device insertion. The authors propose that it may help young women whose risk of developing ovarian cancer is known to be high in deciding whether to have their ovaries removed as a preventative measure. The method of isolating microvesicles from bodily fluids to detect faint cancer signals also may have promise for other difficult-to-detect types of cancer.
Enjoy reading ASBMB Today?
Become a member to receive the print edition four times a year and the digital edition monthly.
Learn moreGet the latest from ASBMB Today
Enter your email address, and we’ll send you a weekly email with recent articles, interviews and more.
Latest in Science
Science highlights or most popular articles

Gaze into the proteomics crystal ball
The 15th International Symposium on Proteomics in the Life Sciences symposium will be held August 17–21 in Cambridge, Massachusetts.

Bacterial enzyme catalyzes body odor compound formation
Researchers identify a skin-resident Staphylococcus hominis dipeptidase involved in creating sulfur-containing secretions. Read more about this recent Journal of Biological Chemistry paper.

Neurobiology of stress and substance use
MOSAIC scholar and proud Latino, Bryan Cruz of Scripps Research Institute studies the neurochemical origins of PTSD-related alcohol use using a multidisciplinary approach.

Pesticide disrupts neuronal potentiation
New research reveals how deltamethrin may disrupt brain development by altering the protein cargo of brain-derived extracellular vesicles. Read more about this recent Molecular & Cellular Proteomics article.

A look into the rice glycoproteome
Researchers mapped posttranslational modifications in Oryza sativa, revealing hundreds of alterations tied to key plant processes. Read more about this recent Molecular & Cellular Proteomics paper.

Proteomic variation in heart tissues
By tracking protein changes in stem cell–derived heart cells, researchers from Cedars-Sinai uncovered surprising diversity — including a potential new cell type — that could reshape how we study and treat heart disease.

